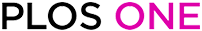Flow chart of patient selection.
Background
It is unclear whether abdominal adiposity has an additional effect on post-stroke outcomes. This study aimed to determine whether waist circumference (WC) is independently associated with clinical outcomes after acute ischemic stroke.
Methods
We enrolled patients with acute ischemic stroke from a multicenter hospital-based stroke registry in Fukuoka, Japan. We measured WC on admission and categorized patients into four groups (Q1–Q4) according to the quartiles in females and males. The clinical outcomes were poor functional outcome (modified Rankin scale score 2–6) and death from any cause. Logistic regression analysis was performed to estimate the odds ratio and 95% confidence interval of the outcomes of interest after adjusting for potential confounding factors, including body mass index (BMI).
Results
A total of 11,989 patients (70.3±12.2 years, females: 36.1%) were included in the analysis. The risk of poor functional outcome significantly decreased for Q2–Q4 (vs. Q1) at discharge and Q2–Q3 (vs. Q1) at 3 months, even after adjusting for potential confounders, including BMI. In contrast, adjustment of BMI eliminated the significant association between WC and all-cause death at discharge and 3 months. The association between high WC and favorable functional outcome was not affected by fasting insulin levels or homeostatic model assessment for insulin resistance and was only found in patients without diabetes (P = 0.02 for heterogeneity).
Conclusions
These findings suggest that abdominal adiposity has an additional impact on post-stroke functional outcome, independent of body weight and insulin action.